Contents
- 1. What is Knee Osteoarthritis? Who is at risk?
- 2. What are the signs of knee osteoarthritis?
- 3. What are the causes of knee osteoarthritis?
- 4. What complications can patients face with knee osteoarthritis?
- 5. How is knee osteoarthritis diagnosed?
- 6. Treatment methods for knee osteoarthritis
- 7. Criteria for Choosing a Suitable Treatment Facility
- 8. Key Considerations for Caring for Patients with Knee Osteoarthritis
- 9. How to Prevent Knee Osteoarthritis Early On
- 10. Frequently Asked Questions (FAQs)
According to a research paper published on NCBI (National Center for Biotechnology Information), knee osteoarthritis is the most commonly diagnosed type of arthritis. Furthermore, the prevalence of this condition is expected to continue rising as average life expectancy increases and obesity rates climb.
1. What is Knee Osteoarthritis? Who is at risk?
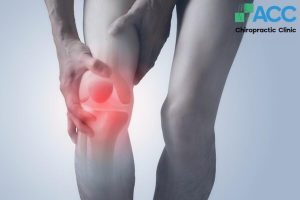
Knee osteoarthritis is a condition characterized by damage to the surface of the joint cartilage. Over time, the cartilage wears down, becoming rough, thin, and losing its elasticity, which leaves the bone ends unprotected. This leads to alterations in the joint surface, increased calcium deposits forming bone spurs (osteophytes), and ultimately results in joint deformity and permanent joint damage.
According to the World Health Organization (WHO), knee osteoarthritis and osteoarthritis in general are most common among the elderly (approximately 70% of patients are over the age of 55). Notably, about 60% of those suffering from osteoarthritis are women.

2. What are the signs of knee osteoarthritis?
General signs of knee osteoarthritis include audible joint noises during movement, swelling or a sensation of edema, and joint stiffness (especially after standing up or sitting for prolonged periods). Furthermore, symptoms vary across different stages as follows:
Stage 1: Minor Osteoarthritis (Grade 1) Symptoms in this stage are usually not apparent. Degeneration is only beginning at a minor level, with potentially slight changes in the joint structure. Cartilage may show minor wear but does not yet cause significant pain or impact activities.
- Signs: Little to no pain; mild joint stiffness; occasional difficulty in bending or straightening the knee.
Stage 2: Mild to Moderate Osteoarthritis (Grade 2) In this stage, cartilage damage becomes more noticeable, and small cracks (fibrillations) may appear. Although the joint shows wear, it remains stable. However, some symptoms start to manifest more clearly.
- Signs: Mild to moderate pain, especially during weight-bearing activities like walking or climbing stairs; morning stiffness; “crepitus” (grating or popping sounds) during movement; discomfort when standing for a long time.
Stage 3: Moderate to Severe Osteoarthritis (Grade 3) Osteoarthritis becomes more serious at this stage, with significant cartilage damage causing the bone ends to come into closer contact. This stage is often accompanied by inflammation, swelling, and distinct pain. The knee’s range of motion may be restricted.
- Signs: Increased pain even at rest; joint inflammation and swelling; difficulty walking or climbing stairs; reduced mobility and flexibility; a feeling of joint “instability” or weakness.
Stage 4: End-stage Osteoarthritis (Grade 4) The joint cartilage is almost completely lost, and the bone ends rub directly against each other, causing extreme pain. Inflammation, swelling, and mobility issues become severe. The joint may lose its function and normal movement capacity entirely.
- Signs: Intense, chronic pain even when stationary; visible joint deformity; severe inflammation; nearly complete loss of mobility, making it difficult to stand, walk, or perform basic daily activities.
3. What are the causes of knee osteoarthritis?
The causes of knee osteoarthritis include aging, being overweight, injuries, etc. Specific reasons are as follows:
- Age: As age increases, the body’s ability to synthesize cartilage declines. Furthermore, after reaching adulthood, chondrocytes (cartilage cells) lose their ability to reproduce and self-regenerate.
- Overweight/Obesity: Excess weight places significant pressure on both knee joints, causing cartilage to wear down and deteriorate rapidly over time. Surveys show that obese women over the age of 40 are six times more likely to develop knee osteoarthritis than those of normal weight. For obese individuals, losing just 5kg can reduce the risk of osteoarthritis and arthritis by half.

- Obesity or Rapid Weight Gain: These conditions cause the musculoskeletal system to be compressed under the body’s weight.
- Gender: Women aged 55 and older are generally at a higher risk of developing arthritis than men. This is due to a weaker anterior cruciate ligament (ACL) and the habit of wearing high heels, which places direct pressure on the cartilage, accelerating the degenerative process.
- Repetitive Knee Stress: Frequently subjecting the knees to high pressure due to work or sports can increase the risk of osteoarthritis.
- Injuries: Sports or occupational injuries can result in fractures of the patella (kneecap), the lower end of the femur, or ligament strains and tears… leading to severe cartilage damage. If not treated early, these injuries can cause joint malalignment, leading to progressive degeneration.
- Genetics: If there is a family history of knee osteoarthritis, there is a higher likelihood that you will also develop the condition.
- Other Risk Factors: (Other causes not mentioned above).
4. What complications can patients face with knee osteoarthritis?
Knee osteoarthritis causes significant discomfort. As the condition worsens, it can lead to more dangerous complications such as:
- Difficulty walking and reduced mobility.
- Joint deformity; lower limbs may become bowed (varus) or knock-kneed (valgus).
- Joint stiffness and muscle atrophy.
- Chondrocalcinosis (calcification of the joint cartilage).
- Disability or paralysis.
On the other hand, knee degeneration can also lead to anxiety or depression, impacting daily life:
- Decreased Productivity: Pain and impaired mobility hinder the ability to concentrate and perform work effectively.
- Sleep Disorders: Persistent pain and swelling prevent restful sleep and make it difficult to find a comfortable position. Continuous insomnia leads to chronic fatigue and lethargy.
- Weight Gain: Pain and stiffness limit movement and exercise, leading to unhealthy weight gain. In turn, this extra weight places further stress on the joints, worsening the condition (a “vicious cycle”).
- Comorbidities: The condition can also contribute to other health issues such as gout, cardiovascular disease, and diabetes, significantly affecting overall health.
5. How is knee osteoarthritis diagnosed?
To accurately diagnose knee osteoarthritis, the doctor will conduct a clinical assessment of the patient’s symptoms combined with diagnostic imaging results. Specifically:
5.1. Symptom-based diagnosis
- Knee Pain: Initially, the pain is dull and intermittent. Gradually, it becomes more severe and persistent. Notably, the pain worsens during cold weather or when barometric pressure drops. At this stage, even a minor movement can cause knee pain that lasts all day.
- Knee Stiffness: This typically occurs in the morning and lasts for about 30 minutes. If the condition worsens, the stiffness will be more prolonged.
- Joint Deformity: Presence of bone spurs, joint malalignment, or synovial herniation.
- Crepitus: Audible grating or popping sounds whenever the joint moves.
- Knee Effusion: Commonly known as “fluid on the knee.”
5.2. Imaging-based diagnosis
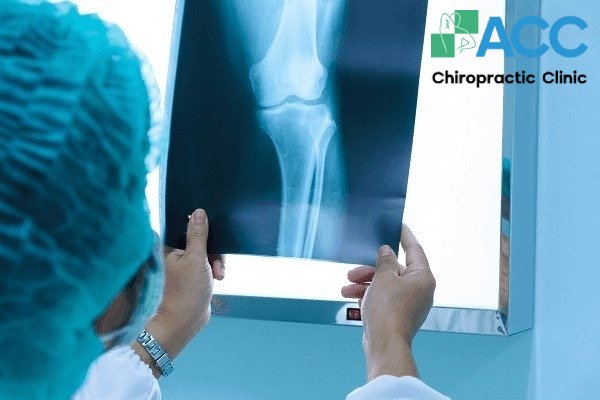
- X-ray: Used to detect signs of joint space narrowing, bone spurs on the shaft and patella (kneecap), increased subchondral bone density, and calcification in the posterior hamstrings.
- Joint Ultrasound: Detects joint effusion, joint space narrowing, bone spurs, and evaluates the thickness of the joint cartilage.
- MRI (Magnetic Resonance Imaging): Provides a 3D view of the joint to detect damage to the cartilage, ligaments, and synovial membrane.
- Arthroscopy: Allows direct observation and precise assessment of the extent of cartilage degeneration, clearly distinguishing it from other joint pathologies.
- Laboratory Tests: Blood tests, biochemistry, and synovial fluid analysis to check white blood cell counts, viscosity, and other markers.
6. Treatment methods for knee osteoarthritis
There are various methods to treat knee degeneration, ranging from conservative care (weight loss, physical therapy, medication, etc.) to surgical intervention. Specifically:
6.1. Non-pharmacological treatments (Non-drug treatments)
- Weight Loss (if overweight): Losing weight helps alleviate the excessive pressure on the knees caused by body mass.
- Therapeutic Exercises for Knee Osteoarthritis: Doctors will prescribe exercises to strengthen the muscles surrounding the knee and flexibility drills to ensure smoother joint movement.
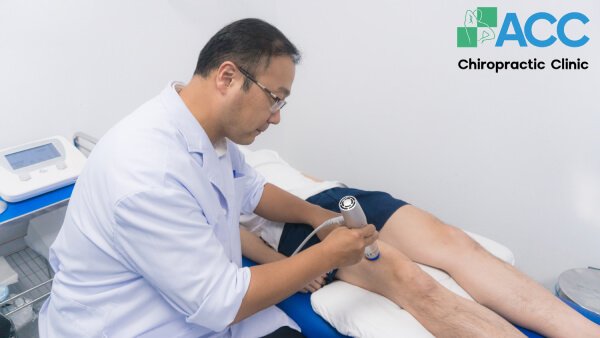
- Physical Therapy for Pain Relief: There are two types of physical therapy: passive and active. In passive therapy, the clinician performs the techniques on the patient, whereas in active therapy, the patient performs the exercises themselves (often as a home exercise program).
- Posture Correction: Patients should avoid squatting or sitting with crossed legs and limit climbing stairs to prevent placing undue stress on the knee joints.
6.2. Pharmacological Treatment (Medication)
- Analgesics and Antipyretics: Acetaminophen (Tydol), used for mild to moderate knee osteoarthritis.
- Non-Steroidal Anti-Inflammatory Drugs (NSAIDs): If Acetaminophen is ineffective, patients may use Naproxen (Aleve) or Ibuprofen (Motrin).
- Topical Medications: Gels such as Voltaren Emulgel applied to the knee 2-3 times daily for rapid local pain relief.
- Symptomatic Slow-Acting Drugs for Osteoarthritis (SYSADOA): Glucosamine, Chondroitin, and Diacerein help improve symptoms and slow disease progression.
- Intra-articular Injections: Corticosteroids or Hyaluronic Acid to provide lubrication, reduce inflammation, and alleviate joint stiffness.
- Herbal Poultices: Natural ingredients (such as wormwood or piper lolot) are minced and applied to the knee as a traditional supportive remedy.
6.3. Surgical Intervention
- Knee Arthroscopy: A minimally invasive procedure using a small endoscope to clean the joint removing cartilage fragments, bone spurs, or inflamed tissue to improve mobility.
- High Tibial Osteotomy (HTO): The surgeon reshapes the tibia (shinbone) or femur to realign the joint axis, shifting weight away from the damaged cartilage to the healthier part of the knee.
- Total Knee Arthroplasty (TKA) or Partial Replacement: When the joint surface is severely damaged, the worn-out parts are replaced with artificial components to restore function and gait.
7. Criteria for Choosing a Suitable Treatment Facility
7.1. Accredited Medical Institutions
Patients should prioritize major hospitals or clinics affiliated with reputable international healthcare groups. These facilities operate under rigorous medical protocols validated by global health organizations, ensuring a standardized diagnostic and treatment process.
7.2. Established Track Record and Clinical Experience
A trustworthy facility typically has nearly 20 years of operation in Vietnam, having treated a vast number of cases ranging from mild to complex. This longevity provides the team with a deep understanding of the unique physical characteristics and lifestyles of Vietnamese patients.
7.3. Qualified Team of Specialists and Doctors
Beyond treatment duration, patients should look for clear professional benchmarks:
- Expatriate Doctors: Formally trained in Chiropractic in developed countries (USA, Canada, France, etc.).
- Clinical Experience: At least 10 years of experience in musculoskeletal and spinal care.
- Specialized Staff: A synchronized team where physical therapists are also professionally certified and highly experienced.
7.4. Medical-Grade Quality Control
Reputable clinics implement strict internal quality control systems, including:
- Comprehensive pre- and post-treatment assessments.
- Continuously updated electronic medical records (EMR).
- Evidence-based protocols targeting the root cause rather than just temporary symptom suppression.
7.5. Personalized Treatment Protocols
The core of effective care lies in Individualized Treatment Plans based on:
- The specific stage of joint degeneration.
- The patient’s age, physical condition, and activity goals.
- Medical history and comorbidities. This approach combines Chiropractic adjustments, Physical Therapy, and specialized rehabilitation to optimize recovery time.
7.6. Long-Term Support and Patient Empowerment
A premier facility focuses on “post-clinic” care:
- Providing customized Home Exercise Programs (HEP).
- Ergonomic counseling for daily activities and workplace posture.
- Regular follow-ups to monitor progress and prevent recurrence, empowering patients to take an active role in their own recovery.
8. Key Considerations for Caring for Patients with Knee Osteoarthritis
When caring for someone with knee degeneration, you can apply cold compresses to reduce swelling and inflammation, prioritize rest, and implement fall prevention measures:
- Cold Therapy: Apply ice packs to alleviate pain and swelling in the knee area.
- Prioritize Rest: Ensure the patient rests, especially after physical activity; provide mobility assistance if needed (crutches, walkers, etc.).
- Fall Prevention: Install raised toilet seats and grab bars, and clear walkways to minimize the risk of tripping or slipping.
- Nutritional Support for Cartilage: Incorporate foods beneficial for joint health, such as fruits, green vegetables, and fatty fish.
Osteoarthritis is essentially a condition characterized by damage to the articular cartilage, accompanied by inflammation and a reduction in synovial fluid. This occurs when the cartilage regeneration process cannot keep pace with the wear and tear over time. Knee osteoarthritis is the most common form, as this joint constantly bears…
9. How to Prevent Knee Osteoarthritis Early On
Without proper joint care, you may unintentionally accelerate the progression of knee degeneration. It is essential to prevent the condition early through simple measures like regular exercise, a balanced diet, and weight management:
- Regular and Correct Exercise: Engage in low-impact sports such as swimming, walking, or cycling. Avoid sudden or high-impact movements.
- Scientific Diet: Maintain a diet rich in calcium and minerals; avoid excessive fats, alcohol, and stimulants that can cause muscle stiffness.
- Weight Management: Maintain a healthy weight to avoid the strain of overweight or obesity.
- Office Ergonomics: Office workers should take a break every 1-2 hours and change positions every 20 minutes to prevent muscle and joint fatigue.
- Daily Massage: Gently massage the knee joints every morning and evening to relax muscles and improve blood circulation.
- Periodic Health Check-ups: Proactively seek knowledge about musculoskeletal conditions and schedule regular screenings.
10. Frequently Asked Questions (FAQs)
Common concerns regarding knee degeneration include:
10.1 Is knee osteoarthritis contagious?
Knee osteoarthritis cannot be transmitted from person to person. However, there is a genetic component, so you should be vigilant if you have a family history of the condition.
10.2 Can people with knee osteoarthritis go cycling?
Yes, but it must be done “scientifically” meaning the intensity, posture, and frequency must be appropriate to support joint movement without placing excessive pressure on the joints.
10.3 Can knee osteoarthritis be fully cured?
As a chronic condition, it cannot be completely “cured” in the traditional sense. However, it can be effectively managed with a low risk of dangerous complications if detected early and treated correctly.
10.4 Should people with knee osteoarthritis take calcium supplements?
To determine if your specific condition requires supplemental calcium, you should consult a doctor. Do not take supplements without a medical prescription to avoid potential health risks.
Knee osteoarthritis is a leading cause of disability if ignored. Therefore, at the first sign of knee abnormalities, seek a medical examination immediately to prevent serious complications.
>> realated posts: