Contents
- 1. The Mechanics of Knee Degeneration
- 2. The 4 Stages of Knee Osteoarthritis (OA)
- 3. Recognizing the Red Flags: Is Your Knee Trying to Tell You Something?
- 4. Why Does It Happen?
- 5. Who is Most at Risk? Identifying the High-Risk Groups
- 6. Is Knee Arthritis Dangerous? The Impact of Delay
- 7. How is Knee Arthritis Diagnosed?
- 8. How is Knee Osteoarthritis Treated?
- 8.1. Weight Management: Lightening the Load
- 8.2. Orthopedic Devices: Structural Support
- 8.3. Medication & Targeted Injections
- 8.4. Acupuncture & Holistic Synergy
- 8.5. Surgery: The Final Resource
- 8.6. Chiropractic Care: Restoring Structural Integrity
- Why Choose ACC Clinic for Your Recovery?
- 8.7. Physiotherapy & Advanced Rehabilitation
- 9. Proactive Prevention: Protecting Your Joints for the Future
- 10. Frequently Asked Questions
Early signs of knee arthritis include pain and stiffness upon waking or when the weather changes. However, many people underestimate and ignore these symptoms, leading to serious consequences.
1. The Mechanics of Knee Degeneration
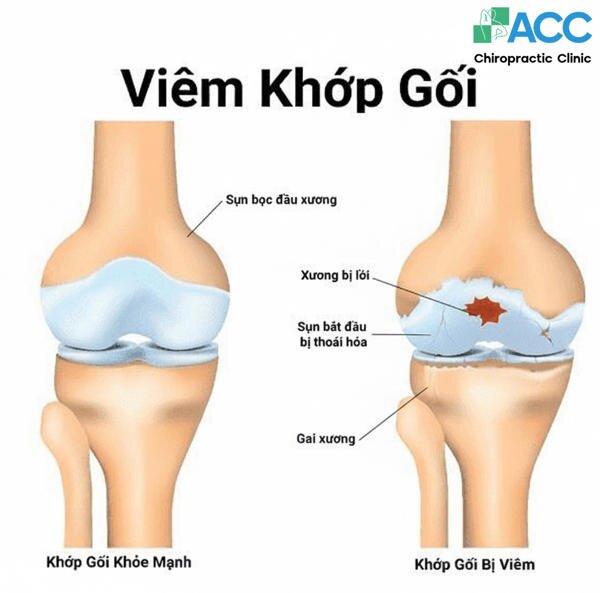
Osteoarthritis of the knee is characterized by the progressive degradation of articular cartilage. When this vital cushioning is compromised, the resulting bone-on-bone friction leads to inflammation, reduced mobility, and chronic pain.
Unfortunately, many cases remain undiagnosed until significant degeneration has occurred. Improper self-treatment further increases the risk of long-term complications. While the prevalence of knee arthritis increases significantly after age 45, clinical awareness and early diagnostic imaging are essential for patients of all ages to prevent irreversible joint damage.
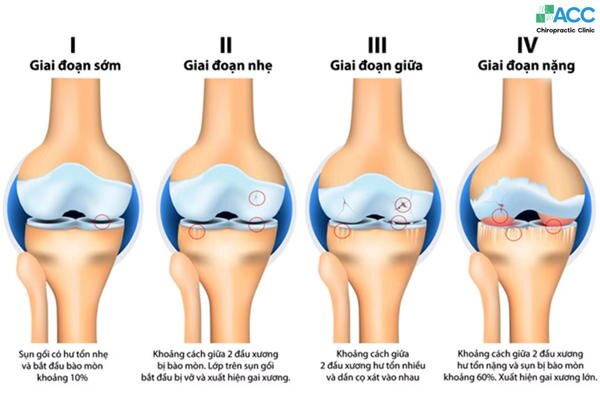
2. The 4 Stages of Knee Osteoarthritis (OA)
- Stage 1: Early (Minor)
At this beginning stage, the joint shows very slight wear. While small bone spurs (osteophytes) may begin to form, the cartilage remains largely intact.
Symptoms: Most people feel no pain or discomfort.
X-ray Findings: Minor bone growths; the joint space appears normal.
- Stage 2: Mild
This is often when patients first notice something is wrong. The diagnostic criteria show more bone spur growth, and the protective cartilage begins to thin, though the bones are not yet rubbing together.
Symptoms: Occasional joint pain, stiffness after sitting for long periods, or “cracking” sounds when walking. These are often dismissed as “fleeting” aches.
X-ray Findings: Visible bone spurs; the joint space remains adequate but shows the start of narrowing.
- Stage 3: Moderate
The damage is now clearly visible. The gap between the bones narrows significantly as the cartilage continues to erode. The joint becomes inflamed, and the synovial fluid (the joint’s natural lubricant) may decrease.
Symptoms: Frequent pain during movement (walking, squatting, or taking stairs) and morning stiffness that takes longer to “warm up.”
X-ray Findings: Significant joint space narrowing; obvious cartilage loss and hardening of the bone (sclerosis).
- Stage 4: Severe
This is the “bone-on-bone” stage. The cartilage is almost completely gone, leaving the bones to rub directly against each other. This leads to chronic inflammation and potential joint deformity.
Symptoms: Intense pain, even at rest. Mobility is severely limited, and the knee may appear “locked” or bowed.
X-ray Findings: Minimal to no joint space; large bone spurs and significant bone-on-bone contact.
3. Recognizing the Red Flags: Is Your Knee Trying to Tell You Something?
Symptoms of knee inflammation rarely appear overnight. They usually start as a whisper, a dull ache, before progressing to a loud, painful shout. Watch for these four typical signs:
- The “Morning Tax” (Pain & Stiffness): Do you need a “warm-up” period? Stiffness immediately upon waking that lasts 10–30 minutes is a classic sign. Often, the joint won’t move smoothly until you’ve massaged it or moved around the house.
- Heat & Swelling: If the skin around your knee feels warm to the touch or looks “puffy,” your body is signaling active inflammation. This is often most noticeable after you’ve been resting or following a nap.
- The Sound of Friction: Healthy joints are silent. If you hear crepitus-that signature cracking, popping, or grinding sound-it’s often caused by loose cartilage fragments or bone-on-bone friction hindering smooth movement.
- Instability & “Locking”: Does your knee ever feel like it’s going to “give out”? Inflammation can lead to muscle weakness or a “locked” sensation where the joint physically resists bending or straightening.
4. Why Does It Happen?
Understanding the Root Causes of Knee Arthritis isn’t just about “getting old.” It is a complex result of lifestyle, biology, and biomechanics.
4.1. The Natural Aging Process.
As we age, our “internal repair kit” slows down. Cartilage loses its elasticity, and the production of synovial fluid (your joint’s natural lubricant) decreases. Think of it like a car engine running on old oil-the parts begin to grind, making inflammation almost inevitable for many adults over 50.
4.2. Underlying Conditions & Biomechanics
Sometimes, the knee is a victim of other issues in the body.
- Condition: How it Affects the Knee
- Osteoarthritis (OA): The “wear and tear” variety. Triggered by aging, previous injuries, or repetitive stress (like frequent squatting).
- Rheumatoid Arthritis (RA): An autoimmune response where the body attacks its own joint lining (synovium), leading to deformity if left untreated.
- Flat Feet (Overpronation): The “Chain Reaction” Cause: When your arches collapse, it forces your legs to rotate inward, placing uneven pressure on the inner knee joint.
4.3. The Impact of Physical Trauma
Whether from a sudden sports pivot, a workplace mishap, or a traffic accident, these injuries change how your knee handles pressure:
- Sprains (Ligament Overstretch): A sprain occurs when the ligaments-the “tough ropes” holding your bones together-are stretched or micro-torn. While not a full rupture, the resulting inflammation, bruising, and warmth can weaken the joint’s stability, forcing the cartilage to work harder.
- Knee Bursitis (The “Cushion” Inflammation): Your knee is equipped with small, fluid-filled sacs called bursae that act as lubricants between bone and soft tissue. An injury can cause these sacs to swell. When the bursa is inflamed, every movement of a tendon or ligament creates friction, leading to significant stiffness and localized pain.
- Dislocations (Joint Misalignment): A dislocation occurs when the bones of the knee joint are forced out of their natural alignment. This is common in high-impact sports and usually involves:
- Patellar Dislocation: The kneecap slips out of its groove.
- Tibiofemoral Dislocation: A more severe injury where the thigh bone and shin bone lose contact.
Why it leads to arthritis: Even after the bone is “popped” back in, the trauma often leaves behind permanent cartilage scarring or loose fragments that act like “sand in a gear,” grinding away at the joint surface.
4.4. Gout: The “Crystal” Factor
Gout is more than just a “big toe” problem. It is a metabolic condition triggered when the kidneys cannot efficiently process purines, leading to a buildup of uric acid in the bloodstream.
How it affects the knee: Over time, this acid solidifies into sharp, needle-like crystals that settle within the joint capsule.
The Damage: These crystals act like “sandpaper” against the smooth cartilage, causing intense inflammation and compressing the sensory nerves. If left untreated, chronic gout can lead to permanent joint erosion and deformity in the knee.
4.5. Overweight and Obesity: The Physics of Pressure
Excess weight is one of the most significant yet most manageable-risk factors for knee arthritis. It impacts the joint in two distinct ways:
- The Multiplier Effect: The knee is a weight-bearing joint. For every 1 pound of body weight you carry, your knees experience 4 pounds of pressure when walking. If you are 20 lbs overweight, your knees are processing an extra 80 lbs of force with every step.
- Chemical Inflammation: Fat tissue isn’t just stored energy; it is metabolically active. It produces proteins (cytokines) that promote systemic inflammation throughout the body, including the joints, which accelerates the breakdown of cartilage.
- The Bottom Line: For those already suffering from knee pain, even a modest weight loss can significantly reduce daily discomfort and slow the progression of degeneration.

5. Who is Most at Risk? Identifying the High-Risk Groups
While anyone can develop joint issues, certain groups are statistically more likely to experience the breakdown of knee cartilage.
5.1. The Biological Factors
- The Golden Years (60+): Naturally, the risk increases as the body’s regenerative capabilities slow down. Most patients start to see significant symptoms after the age of 60.
- The Gender Gap: Women are disproportionately affected. Statistics show that while 10% of men over 60 suffer from knee arthritis, that number jumps to 13% for women, often due to hormonal changes and different hip-to-knee biomechanics.
- Genetics: If your parents or siblings have struggled with chronic joint pain, you may have an inherited predisposition to cartilage weakness.
5.2. The Lifestyle & Occupational Factors
- Manual Laborers: Your job can “weather” your joints. High-risk activities include:
- Standing for more than 2 hours a day.
- Carrying heavy loads or frequent heavy lifting.
- Repetitive bending, kneeling, or walking long distances (over 3 km/day).
- Athletes & Previous Injuries: High-impact sports often lead to “hidden” damage. Even if a cartilage tear, fracture, or patellar dislocation happened years ago, it significantly raises the risk of arthritis later in life.
- Weight & Inactivity: A sedentary lifestyle combined with excess weight creates a “double hit”-the joints are weakened by lack of movement while simultaneously being crushed by extra pressure.
5.3. The “Stress” Connection
Modern research shows that frequent stress is more than just a mental burden. Chronic stress triggers the constant production of inflammatory chemicals in the body. This can weaken the immune system and accelerate the breakdown of joint tissue, turning “normal” aches into chronic arthritis.
6. Is Knee Arthritis Dangerous? The Impact of Delay
While knee arthritis is not a life-threatening condition, it is a life-altering one. Ignoring the symptoms doesn’t just mean “living with pain”-it often leads to a progressive loss of independence.
6.1. The Reality of the Condition
- 80% of Patients: Experience significant limitations in normal movements (climbing stairs, walking, or standing).
- 20% of Patients: Face a severe decline in quality of life, including chronic insomnia due to night pain, decreased work productivity, and a higher risk of depression.
6.2. The Risk of Permanent Disability
Delaying professional treatment is a gamble with your mobility. Without intervention, knee inflammation can lead to:
- Muscle Atrophy: Because it hurts to move, muscles around the knee weaken and shrink, making the joint even less stable.
- Joint Deformity: The legs may begin to bow (O-shape) or knock (X-shape) as the bone structure changes.
- Permanent Loss of Mobility: In extreme cases, the joint can “fuse” or become so unstable that the patient can no longer walk without assistance.
6.3. When to Seek Immediate Medical Attention
Do not wait for the “perfect time” to see a specialist. Schedule an appointment immediately if you experience:
- Weight-Bearing Failure: You cannot put any weight on the leg or feel “unsteady” standing.
- Visible Inflammation: The joint is swollen, red, and hot to the touch.
- Mechanical Locking: You physically cannot bend or straighten your leg, often accompanied by a loud “crack.”
- Systemic Symptoms: Joint pain paired with a high fever or unusual fatigue (this could indicate an infection).
- Visual Abnormality: One knee looks significantly different in shape or size compared to the other.
- The 3-Day Rule: Pain that shows zero improvement after 3–5 days of rest and home care.
7. How is Knee Arthritis Diagnosed?
A proper diagnosis is like a roadmap-it tells us exactly where the damage is and how to fix it. This process involves two main phases:
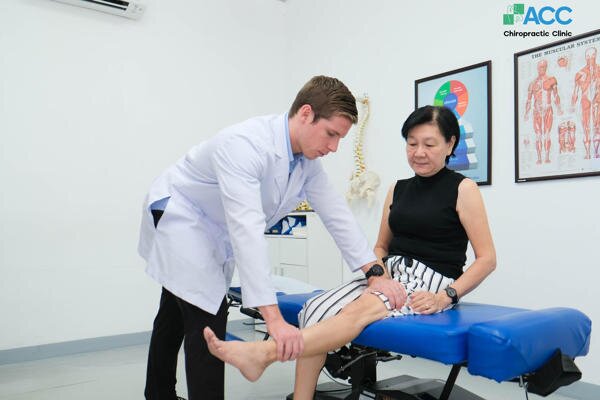
7.1. Clinical Physical Examination
Your doctor acts as a “detective” to understand your specific pain profile. This includes:
- Symptom History: Discussing your pain triggers, the “morning tax” (stiffness), and any clicking sounds.
- Functional Testing: Observing your gait (how you walk) and checking your Range of Motion (ROM)-how far you can comfortably bend and straighten the leg.
- Palpation & Stability: The doctor will feel for warmth and swelling and perform specific maneuvers to check if your ligaments are still providing a stable foundation.
7.2. Diagnostic Imaging: Looking Beneath the Surface
Physical exams tell us where it hurts, but imaging tells us why. Each technology serves a specific purpose in the diagnostic “toolkit”:
- X-ray (The Baseline): This is usually the first step. It is excellent for spotting bone-on-bone contact, narrowing joint spaces, and the development of bone spurs.
- MRI Scan (The Deep Dive): Unlike X-rays, MRIs capture the “soft” parts of your knee. It is the gold standard for identifying cartilage tears, ligament damage, and early-stage inflammation of the synovial lining.
- Ultrasound: This is a quick, non-invasive way to check for joint effusion (fluid buildup) and real-time inflammation in the tendons around the knee.
- CT Scan: Reserved for complex cases, a CT scan provides a 3D view of the bone structure, helping doctors detect tiny micro-fractures or bone lesions that a standard X-ray might miss.
8. How is Knee Osteoarthritis Treated?
Modern treatment focuses on Multimodal Care-combining different strategies to reduce pain, restore function, and avoid or delay surgery.
8.1. Weight Management: Lightening the Load
As mentioned earlier, your knees feel 4lbs of pressure for every 1lb of body weight. Reducing your weight is the most effective way to “naturally” decrease joint wear.
The Benefit: Even a 5–10% weight loss has been clinically proven to significantly reduce pain scores and improve mobility without the need for medication.
8.2. Orthopedic Devices: Structural Support
When a joint is damaged, it often becomes misaligned. Orthopedic tools help “re-balance” your weight:
Knee Braces: Specifically, “unloader” braces shift pressure from the damaged side of the knee to the healthier side.
Medical Grade Insoles: For those with flat feet, custom orthotics correct the foundation. By supporting the arch, they prevent the knee from rotating inward, which stops the uneven grinding of cartilage.
8.3. Medication & Targeted Injections
Medication is often used to manage symptoms so that you can participate in more active therapies like physical therapy.
- Oral Medications: Options include Acetaminophen for mild pain or NSAIDs (like Ibuprofen) and COX-2 inhibitors to bring down active swelling.
- Injections (Advanced Therapy):
- Corticosteroids: High-potency anti-inflammatories for immediate, short-term relief.
- Hyaluronic Acid (Lubricant): Often called “synovial fluid injections,” this helps “grease” the joint.
- PRP (Platelet-Rich Plasma): Uses the patient’s own blood cells to stimulate a healing response in the damaged tissues.
8.4. Acupuncture & Holistic Synergy
Acupuncture serves as a powerful natural analgesic. By precisely stimulating specific meridians around the knee, this therapy triggers the release of endorphins and improves micro-circulation to the damaged area.
The Benefit: It reduces systemic inflammation and “wakes up” the body’s self-healing mechanisms.
Enhanced Results: For patients with severe stiffness, acupuncture is often combined with medical massage or thread embedding to break down scar tissue and restore fluid, flexible movement.
8.5. Surgery: The Final Resource
Surgery is considered only when the arthritis has reached Stage 4, and the joint no longer responds to conservative care.
Procedures: Options range from minimally invasive arthroscopy (cleaning the joint) to total knee replacement.
The Caveats: While effective for some, surgery is an invasive process with inherent risks such as infection, blood clots, and a grueling rehabilitation period that can last months. It is essential to exhaust non-surgical options before committing to the operating table.
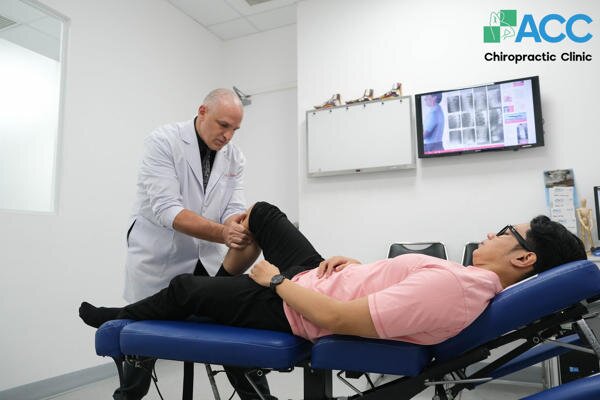
8.6. Chiropractic Care: Restoring Structural Integrity
Chiropractic treatment is increasingly recognized as a leading non-invasive solution because it addresses the mechanical root cause of the pain rather than just masking the symptoms.
How it Works: The core principle involves the precise realignment of the joint and spinal structures. When the knee or pelvis is “off-track,” it places uneven pressure on the nerves and cartilage. Chiropractic adjustments return these structures to their natural positions, immediately decompressing the nervous system and reducing pain.
Long-Term Goal: By restoring proper biomechanics, this therapy helps prevent the recurrence of inflammation, all without the use of drugs or the risks of surgery.
Why Choose ACC Clinic for Your Recovery?
As a pioneer in Chiropractic care in Vietnam since 2006, ACC Clinic, now a proud member of the FV Group, combines international expertise with world-class healthcare standards.
Elite Medical Team: Our staff is comprised of 100% foreign doctors with over 20 years of specialized experience in musculoskeletal health.
Safety & Precision: We utilize advanced diagnostic tools to ensure every adjustment is tailored to the patient’s specific stage of arthritis, whether they are a young athlete or a senior citizen.
Integrated Care: At ACC, we don’t just “adjust”; we provide a comprehensive ecosystem of care, combining Chiropractic with specialized physiotherapy and medical-grade orthotics to ensure your “Expert in Motion” status is restored.
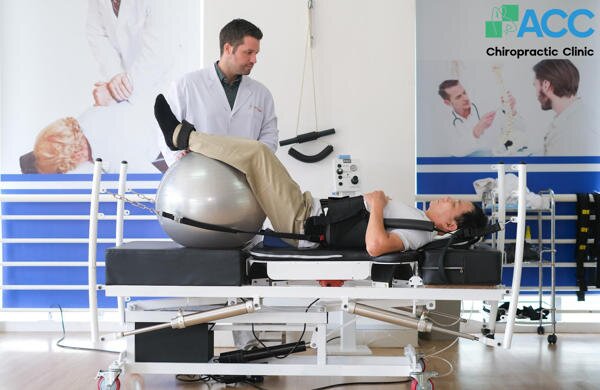
8.7. Physiotherapy & Advanced Rehabilitation
At ACC Clinic, we believe that reducing pain is only half the battle; the other half is restoring the joint’s ability to heal and function. Our physiotherapy programs are designed to accelerate cartilage recovery and strengthen the supporting structures of the knee.
8.7.1. State-of-the-Art Healing Technology
We utilize a suite of advanced equipment, among the most modern in Asia, to target inflammation at a cellular level:
- Class IV Laser Therapy: This high-power laser penetrates deep into the joint tissue to stimulate cellular regeneration and provide rapid pain relief.
- Shockwave Therapy: Using acoustic waves, this treatment breaks down calcified tissue and stimulates blood flow to areas where the body’s natural healing has stalled.
- DTS Spinal Traction & Decompression: While often used for the spine, our advanced decompression technology helps restore overall musculoskeletal balance, ensuring that the hips and lower back aren’t placing secondary stress on your knees.
8.7.2. Targeted Functional Rehabilitation
Beyond the technology, our specialists guide you through a customized exercise regimen. The goal is to move from passive treatment to active strength:
- Muscle Strengthening: We focus on the quadriceps and hamstrings. Stronger thigh muscles act as “natural shock absorbers,” taking the pressure off the joint itself.
- Corrective Technique: Our doctors ensure every movement is performed with precise form. This improves your Range of Motion (ROM) and prevents the “compensation injuries” that occur when you favor one leg over the other.
- Proprioception Training: Exercises designed to improve your balance and joint awareness, reducing the risk of future falls or twists.
9. Proactive Prevention: Protecting Your Joints for the Future
Knee arthritis may be common, but it is not inevitable. By making intentional lifestyle adjustments today, you can significantly delay or even prevent the onset of cartilage degeneration.
9.1. Weight Management: Your Knees’ Best Ally
Maintaining a healthy weight is the single most effective way to protect your knees. As the primary weight-bearing joints, your knees benefit immediately from even modest weight loss, which reduces the daily “grinding” force on the cartilage.
9.2. Injury Prevention & Workplace Safety
A single traumatic injury can lead to arthritis years later. Protect yourself by:
- Lifting Smarter: Avoid carrying excessively heavy loads alone. When you must lift, use your legs, not your back or knees.
- Fall Prevention: Ensure your home and workspace are well-lit and free of tripping hazards.
- Protective Gear: Use high-quality knee pads during high-risk sports or occupations that require frequent kneeling.
9.3. The “Joint-First” Diet
Nutrition is the fuel your body uses to repair tissue. Focus on a menu that nourishes cartilage from the inside out:
- The “Build” List: Prioritize Calcium and Vitamin D for bone density, Vitamin C and K for cartilage repair, and Omega-3 fatty acids (found in salmon and walnuts) to naturally dampen inflammation.
- The “Avoid” List: Minimize refined sugars, red meat, excessive salt, and processed carbohydrates, as these are known triggers for systemic joint inflammation.
10. Frequently Asked Questions
10.1. Can knee arthritis be completely cured?
Knee arthritis is a chronic, degenerative condition, which means there is no “magic pill” to reverse 100% of the cartilage loss. However, this does not mean you are destined for a life of pain. Proper treatment—especially non-invasive therapies like those at ACC Clinic—can effectively stop the progression of the disease, manage pain without drugs, and restore stable mobility. The goal is to move the joint from a state of “degeneration” to a state of “stabilization.”
10.2. Can inflammation in one knee “spread” to the other?
Knee arthritis is not a contagious infection, so it cannot “spread” biologically. However, it often becomes a bilateral issue due to compensation. When your left knee hurts, you naturally shift your weight to your right side to find relief. This uneven mechanical pressure forces the “healthy” knee to do twice the work, which can rapidly accelerate wear and tear on that side. This is why we focus on total body alignment to ensure both knees are protected.
10.3. Should I keep walking if my knees hurt?
Yes, but with caution. Movement is life for a joint. * The Benefit: For those in the early to moderate stages, gentle walking stimulates the production of synovial fluid, which “greases” the joint and delivers nutrients to the cartilage.
The Warning: If you are in an acute inflammatory phase (where the knee is visibly swollen, red, or hot), you should rest. Pushing through severe pain during a flare-up can cause further tissue damage. Once the swelling subsides, you should resume low-impact movement under the guidance of a specialist.
Take Action Today: Don’t Let the Pain Define You
Knee arthritis is a progressive journey. If left untreated, the “quiet aches” of today can become the “permanent disability” of tomorrow. By seeking early, correct treatment, you aren’t just saving yourself from pain—you are saving your time, your independence, and your future quality of life.
Expert in Motions. Do It Right, No Pain Left.
>> Read more:





